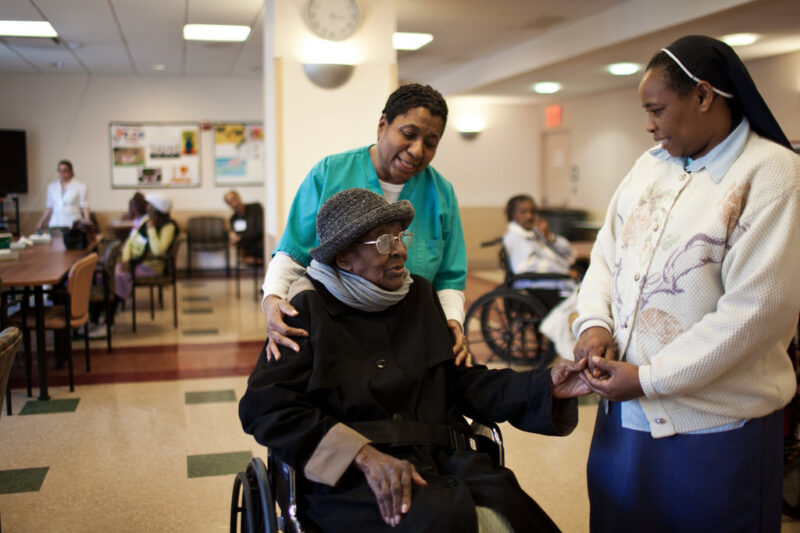Nursing home care is expensive. Even when costs are mediated by insurance, Medicare, or Medicaid, paying for long-term care for an elderly loved one can involve significant costs. Thus, when family members place an elderly loved one in a nursing home, they are hoping that the money they spend will provide optimal care. They read brochures which promise active engagement with their loved ones, care by skilled and experienced professionals, and helpful assistance in case of an emergency. In many facilities across the United States, this is exactly what happens. Older people continue living their lives safely and with good care.
Yet this is not always the case. One important way to avoid the horrors of poor senior care in nursing homes is to inquire about, demand, and support higher staff-to-resident ratios.
Staff-to-Resident Ratios
A staff-to-resident ratio is much like a student-to-teacher ratio. Student-to-teacher ratios are often used to measure whether or not students get sufficient individual attention in the classroom. Staff-to-resident ratios are similar. The more residents have access to personalized care, the better off they will be. They will be more likely to get help in an emergency, have satisfying social interactions, and experience healthy aging. However, if staff numbers are much smaller than resident numbers, dangers arise.
Staff members may be too busy (often during long, eight-hours-plus shifts) to ensure that every senior in their care gets enough physical exercise or is shifted to new positions. If this is the case, residents can experience bed sores, muscle deterioration, stiffness, and more. Insufficient staff numbers also mean high employee turnover and a constant state of stress for staff members who stay. This may mean that an elderly person has a high risk of having someone whose training is less than ideal. Worse yet, residents may be cared for by someone who is exhausted and overworked. Either situation is unacceptable and can lead to serious consequences to an elderly person’s health.
Factors that influence these ratios
The three main factors affecting the ratios of nursing home staff to nursing home residents are money, transparency, and regulation. The easiest to identify is regulation.
Nursing homes adhere to more rigorous national standards than assisted living facilities. They are required to have more licensing (and licensed workers) in their facilities. If a nursing home is certified by Medicare or Medicaid, it must adhere to certain guidelines as far as staff go. The requirements for nurses are most stringent. According to federal law, a nursing home is compliant only if it has RNs (Registered Nurses) and/or LPNs (Licensed Practical Nurses) on duty at all times. However, according to a website on Elder Law, there are no requirements for specific numbers of other health care aides.
Living up to standards
Writing for PBS, Thompson and Jones note that the Centers for Medicare and Medicaid Services (CMS) have a treasure trove of data on nursing homes in the United States. The authors note that this data is accessible through the websites Nursing Home Compare and Nursing Home Inspect. These are good sites for family members to check when selecting or monitoring a nursing home. There are several readily accessible avenues for reporting poor policies and practices in any particular nursing home too.
Yet a nursing home that only lives up to the federal standards is giving residents less than optimal care. Fortunately, most state standards impose greater requirements. However, it is still true that understaffing is a widespread problem in nursing homes. The website ElderLawAnswers has released information on the subject. The website noted that CMS recommendations for staff-to-residents ratios are rarely met.
Can’t ignore the cost
Money is another factor. Often, the seniors with the most money can access facilities which have better resident-to-staff ratios. This higher cost usually means enough employees to assist residents properly. Conversely, low-income seniors tend to have to take what they can get, which means risking poor care.
Perhaps the biggest factors in identifying a healthy staff-to-resident ratio is transparency and accountability. Family members do well to get all facts and figures about a prospective nursing home on paper. They are wise to inquire about staff-to-resident ratios before they enter the facility. They should check during visits to see if those numbers seem viable and how much they vary according to time.
Brochures often cite the day ratios, which may show reasonably robust staffing. However, these ratios can change radically at night. Some facilities lower their ratios when residents are in bed for the night. This may leave them short-handed during emergencies such as fires or gas leaks. If a facility refuses to disclose the information, family members should be leery. Caution is called for too if representatives simply state that the numbers vary in the evening hours. A major red flag for families is if a nursing home cannot even produce a staff-to-resident ratio.
Time is the silent factor
Staff-to-resident ratios may be deceiving. What really counts is time. How much one-on-one, focused, professional care does an elderly loved one receives each day? Is the person in activities that keep him or her engaged? Does the staff reposition residents enough to prevent pressure ulcers? Are they getting necessary hygiene assistance? Does the staff appropriately handle medication?
These aspects of care are often reflected in the staff-to-resident ratios of nursing homes. It is important to check these specifics in order to ensure that elderly loved ones are in good hands.
Sources
ElderLawAnswers.com. What Nursing Home Staff Levels Are Required? ElderLawAnswers.com, May 1, 2013. Available at http://www.elderlawanswers.com/what-nursing-home-staff-levels-are-required-6496. Retrieved September 5, 2016.
Thompson, A. C., and Jones, J. (July 31, 2013). Life & Death in Assisted Living: “A Sinking Ship.” PBS.org and ProPublica, Available at http://www.pbs.org/wgbh/frontline/article/life-death-in-assisted-living-a-sinking-ship/. Retrieved September 5, 2016.